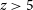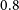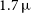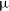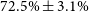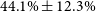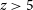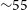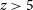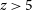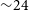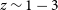16 results
SkyHopper mission science case I: Identification of high redshift Gamma-Ray Bursts through space-based near-infrared afterglow observations
- M. Thomas, M. Trenti, J. Greiner, M. Skrutskie, Duncan A. Forbes, S. Klose, K. J. Mack, R. Mearns, B. Metha, E. Skafidas, G. Tagliaferri, N. Tanvir
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 39 / 2022
- Published online by Cambridge University Press:
- 05 August 2022, e032
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Long-duration gamma-ray burst (GRB) afterglow observations offer cutting-edge opportunities to characterise the star formation history of the Universe back to the epoch of reionisation, and to measure the chemical composition of interstellar and intergalactic gas through absorption spectroscopy. The main barrier to progress is the low efficiency in rapidly and confidently identifying which bursts are high redshift (
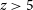 $z > 5$
) candidates before they fade, as this requires low-latency follow-up observations at near-infrared wavelengths (or longer) to determine a reliable photometric redshift estimate. Since no current or planned gamma-ray observatories carry near-infrared telescopes on-board, complementary facilities are needed. So far this task has been performed by instruments on the ground, but sky visibility and weather constraints limit the number of GRB targets that can be observed and the speed at which follow-up is possible. In this work we develop a Monte Carlo simulation framework to investigate an alternative approach based on the use of a rapid-response near-infrared nano-satellite, capable of simultaneous imaging in four bands from
$z > 5$
) candidates before they fade, as this requires low-latency follow-up observations at near-infrared wavelengths (or longer) to determine a reliable photometric redshift estimate. Since no current or planned gamma-ray observatories carry near-infrared telescopes on-board, complementary facilities are needed. So far this task has been performed by instruments on the ground, but sky visibility and weather constraints limit the number of GRB targets that can be observed and the speed at which follow-up is possible. In this work we develop a Monte Carlo simulation framework to investigate an alternative approach based on the use of a rapid-response near-infrared nano-satellite, capable of simultaneous imaging in four bands from
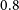 $0.8$
to
$0.8$
to
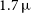 $1.7\,\unicode{x03BC}$
m (a mission concept called SkyHopper). Using as reference a sample of 88 afterglows observed with the GROND instrument on the MPG/ESO telescope, we find that such a nano-satellite is capable of detecting in the H-band (1.6
$1.7\,\unicode{x03BC}$
m (a mission concept called SkyHopper). Using as reference a sample of 88 afterglows observed with the GROND instrument on the MPG/ESO telescope, we find that such a nano-satellite is capable of detecting in the H-band (1.6
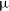 $\unicode{x03BC}$
m)
$\unicode{x03BC}$
m)
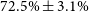 $72.5\% \pm 3.1\%$
of GRBs concurrently observable with the Swift satellite via its UVOT instrument (and
$72.5\% \pm 3.1\%$
of GRBs concurrently observable with the Swift satellite via its UVOT instrument (and
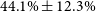 $44.1\% \pm 12.3\%$
of high redshift (
$44.1\% \pm 12.3\%$
of high redshift (
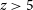 $z>5$
) GRBs) within 60 min of the GRB prompt emission. This corresponds to detecting
$z>5$
) GRBs) within 60 min of the GRB prompt emission. This corresponds to detecting
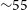 ${\sim}55$
GRB afterglows per year, of which 1–3 have
${\sim}55$
GRB afterglows per year, of which 1–3 have
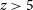 $z > 5$
. These rates represent a substantial contribution to the field of high-z GRB science, as only 23
$z > 5$
. These rates represent a substantial contribution to the field of high-z GRB science, as only 23
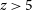 $z > 5$
GRBs have been collectively discovered by the entire astronomical community over the last
$z > 5$
GRBs have been collectively discovered by the entire astronomical community over the last
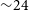 ${\sim}24$
yr. Future discoveries are critically needed to take advantage of next generation follow-up spectroscopic facilities such as 30m-class ground telescopes and the James Webb Space Telescope. Furthermore, a systematic space-based follow-up of afterglows in the near-infrared will offer new insight on the population of dusty (‘dark’) GRBs which are primarily found at cosmic noon (
${\sim}24$
yr. Future discoveries are critically needed to take advantage of next generation follow-up spectroscopic facilities such as 30m-class ground telescopes and the James Webb Space Telescope. Furthermore, a systematic space-based follow-up of afterglows in the near-infrared will offer new insight on the population of dusty (‘dark’) GRBs which are primarily found at cosmic noon (
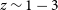 $z\sim 1-3$
). Additionally, we find that launching a mini-constellation of 3 near-infrared nano-satellites would increase the detection fraction of afterglows to
$z\sim 1-3$
). Additionally, we find that launching a mini-constellation of 3 near-infrared nano-satellites would increase the detection fraction of afterglows to
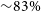 ${\sim}83\%$
and substantially reduce the latency in the photometric redshift determination.
${\sim}83\%$
and substantially reduce the latency in the photometric redshift determination.
The Hierarchical Taxonomy of Psychopathology (HiTOP) in psychiatric practice and research
- Roman Kotov, David C. Cicero, Christopher C. Conway, Colin G. DeYoung, Alexandre Dombrovski, Nicholas R. Eaton, Michael B. First, Miriam K. Forbes, Steven E. Hyman, Katherine G. Jonas, Robert F. Krueger, Robert D. Latzman, James J. Li, Brady D. Nelson, Darrel A. Regier, Craig Rodriguez-Seijas, Camilo J. Ruggero, Leonard J. Simms, Andrew E. Skodol, Irwin D. Waldman, Monika A. Waszczuk, David Watson, Thomas A. Widiger, Sylia Wilson, Aidan G. C. Wright
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 9 / July 2022
- Published online by Cambridge University Press:
- 02 June 2022, pp. 1666-1678
-
- Article
- Export citation
-
The Hierarchical Taxonomy of Psychopathology (HiTOP) has emerged out of the quantitative approach to psychiatric nosology. This approach identifies psychopathology constructs based on patterns of co-variation among signs and symptoms. The initial HiTOP model, which was published in 2017, is based on a large literature that spans decades of research. HiTOP is a living model that undergoes revision as new data become available. Here we discuss advantages and practical considerations of using this system in psychiatric practice and research. We especially highlight limitations of HiTOP and ongoing efforts to address them. We describe differences and similarities between HiTOP and existing diagnostic systems. Next, we review the types of evidence that informed development of HiTOP, including populations in which it has been studied and data on its validity. The paper also describes how HiTOP can facilitate research on genetic and environmental causes of psychopathology as well as the search for neurobiologic mechanisms and novel treatments. Furthermore, we consider implications for public health programs and prevention of mental disorders. We also review data on clinical utility and illustrate clinical application of HiTOP. Importantly, the model is based on measures and practices that are already used widely in clinical settings. HiTOP offers a way to organize and formalize these techniques. This model already can contribute to progress in psychiatry and complement traditional nosologies. Moreover, HiTOP seeks to facilitate research on linkages between phenotypes and biological processes, which may enable construction of a system that encompasses both biomarkers and precise clinical description.
Transjugular venous approach for Piccolo patent ductus arteriosus closure in a 1.4 kg infant
- Christopher Herron, Thomas J. Forbes, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 32 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 06 December 2021, pp. 111-112
-
- Article
- Export citation
-
Transfemoral venous approach is the standard method for transcatheter patent ductus arteriosus closure using the Amplatzer Piccolo patent ductus arteriosus occluder in small infants. We report a 1.4 kg infant who underwent transcatheter Piccolo patent ductus arteriosus closure. Transjugular venous approach was taken due to the unexpected finding of interrupted inferior vena cava.
Pericardiocentesis in children: 20-year experience at a tertiary children’s hospital
- Part of
- Christopher Herron, Thomas J. Forbes, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 32 / Issue 4 / April 2022
- Published online by Cambridge University Press:
- 26 July 2021, pp. 606-611
-
- Article
- Export citation
-
Background:
Pericardiocentesis is the invasive percutaneous procedure for acute and chronic excessive accumulation of pericardial fluid. There is a paucity of data on the effectiveness and safety of pericardiocentesis in children.
Objectives:To evaluate the effectiveness and safety of pericardiocentesis and factors associated with acute procedural failure and adverse events.
Methods:This was a single-centered retrospective study to describe all the children aged ≤20 years who underwent pericardiocentesis. Data on demographics, etiologies of pericardial effusion, and repeat intervention at follow-up were collected.
Results:A total of 127 patients underwent 153 pericardiocentesis. The median age was 6.5 years (1 day–20 years) with weight of 17 kg (0.5–125). Most common etiology was post-pericardiotomy syndrome (n = 56, 44%), followed by infectious (12%), malignant (10%), and iatrogenic (9%). Pericardiocentesis was performed more commonly in the catheterisation laboratory (n = 86, 59%). Concurrent pericardial drain placement was performed in 67 patients (53%). Acute procedural success was 92% (141/153). Repeat intervention was performed in 33 patients (22%). The incidence of adverse events was 4.6% (7/153): hemopericardium requiring emergent surgery (n = 2); hemopericardium with hypotension (n = 2); seizure with anesthesia induction (n = 1); and right ventricle puncture with needle (n = 2). Pericardiocentesis at the bedside had a higher rate of acute procedural failure than that in the catheterisation lab (17 versus 1%, p < 0.01). No identifiable risk factors were associated with adverse events.
Conclusions:Pericardiocentesis was life-saving in children with its high effectiveness and safety even in urgent situations. Although initial pericardiocentesis was effective, one of five patients required re-intervention for recurrent pericardial effusion.
Membranous septal aneurysm causing severe right ventricular outflow obstruction in an adult with trisomy 18
- Christopher Herron, Thomas J Forbes, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 14 May 2021, pp. 1498-1499
-
- Article
- Export citation
-
Membranous ventricular septal aneurysm is a known entity but rarely causes severe right ventricular outflow obstruction. We report a 40-year-old female with trisomy 18 who developed severe right ventricular outflow obstruction caused by an enormous membranous septal aneurysm associated with unrepaired inlet ventricular septal defect with perimembranous extension.
Single center experience of pediatric percutaneous balloon pericardiotomy
- Christopher Herron, Thomas J. Forbes, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 2 / February 2021
- Published online by Cambridge University Press:
- 03 November 2020, pp. 212-215
-
- Article
- Export citation
-
Background:
Percutaneous balloon pericardiotomy is a percutaneous procedure that creates a window in the parietal pericardium by balloon dilation. The use of percutaneous balloon pericardiotomy has not been reported well in children.
Objectives:The objective of this study was to describe the single centre experience of percutaneous balloon pericardiotomy in children.
Methods:This was a retrospective study to describe all the children aged <20 years undergoing percutaneous balloon pericardiotomy during an 18-year period (2001–2019). Patient characteristics, technical and ultimate procedural success, and repeat interventions were collected.
Results:A total of 13 percutaneous balloon pericardiotomy’s were performed in 11 children at the median age of 12 years (range 1.8–19). The etiologies of pericardial effusion were post-pericardiotomy syndrome (n = 4), restrictive cardiomyopathy (n = 1), autoimmune diseases (n = 3), malignancy (n = 2), and idiopathic (n = 1). Two patients received two percutaneous balloon pericardiotomy. The technical success of percutaneous balloon pericardiotomy was 100% with no acute adverse events (balloon rupture or local bleeding). Five (45%) required re-intervention and ultimately three required a surgical pericardial window 6 to 35 days after the percutaneous balloon pericardiotomy. As a result, ultimate procedural success rate was 73% (8/11).
Conclusion:Percutaneous balloon pericardiotomy was performed safely with high technical success in children. Percutaneous balloon pericardiotomy may be considered for recurrent and persistent pericardial effusion, before considering a surgical pericardial window.
Saccular “Cauliflower” aneurysm of coarctation of aorta: a hybrid management
- Neha Bansal, Thomas J. Forbes, Sanjeev Aggarwal
-
- Journal:
- Cardiology in the Young / Volume 30 / Issue 9 / September 2020
- Published online by Cambridge University Press:
- 03 August 2020, pp. 1360-1362
-
- Article
- Export citation
-
Aneurysm formation around the site of coarctation of aortic arch is a well-recognised complication of untreated coarctation and is associated with an increased risk of aortic rupture and mortality. We present a rare case in a teenage girl with the combination of significant aortic arch coarctation, a “cauliflower-like” saccular aneurysm, and stenosis at the origin of the left subclavian artery. She was successfully managed with a hybrid approach, which is a combination of an endovascular surgical repair (a bypass graft placement from left carotid artery to subclavian artery by a vascular surgeon) and a transcatheter covered stent placement across the stenosis and aneurysm. This case highlights the successful role of a hybrid approach in patient’s who present with a combination of coarctation of the aorta and aortic arch aneurysms. This approach avoids the conventional surgical aortoplasty, which carries a higher mortality and morbidity risk in teenage patients.
Recurrent infective endocarditis in a patient after a second Melody valve placement
- Daiji Takajo, Thomas J. Forbes, Sanjeev Aggarwal
-
- Journal:
- Cardiology in the Young / Volume 30 / Issue 7 / July 2020
- Published online by Cambridge University Press:
- 05 June 2020, pp. 1050-1051
-
- Article
- Export citation
-
A 16-year-old Caucasian male was diagnosed with recurrent infective endocarditis associated with his second Melody valve placed inside a previously treated infected Melody valve. The replacement of Melody valve after the first infective endocarditis episode might increase the risk of the second episode of infective endocarditis.
Catheter-directed therapy for acute pulmonary embolism in children
- Jyothsna Akam-Venkata, Thomas J. Forbes, Theodore Schreiber, Amir Kaki, Mahir Elder, Daniel R. Turner, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 29 / Issue 3 / March 2019
- Published online by Cambridge University Press:
- 21 December 2018, pp. 263-269
-
- Article
- Export citation
-
Background
Acute pulmonary embolism is a life-threatening condition and rarely occurs in children. In adults, catheter-directed therapy emerges as a potentially safer and effective therapeutic option. However, there is a paucity of data on the safety and efficacy of catheter-directed therapy for pulmonary embolism in children. We report a single-centred experience of catheter-directed therapy for acute pulmonary embolism in children.
MethodsThis is a retrospective study of children who had no CHD and underwent catheter-directed therapy at Detroit Medical Center during a 12-year period from 2005 to 2017. Demographic and clinical data associated with pulmonary embolism were collected along with the outcome.
ResultsA total of nine patients of median age 16 years with the range from 12 to 20 received catheter-directed therapy for sub-massive (n = 6) and massive pulmonary embolism (n = 3). Among nine patients, one patient received Angiojet thrombectomy and balloon angioplasty, whereas eight patients received catheter-directed thrombolysis using tissue plasminogen activator through infusion catheters (n = 3) or EkoSonic ultrasound-accelerated thrombolysis system (n = 5). In four out of five patients treated with EkoSonic, significant clinical improvement was noticed within 24 hours. Among seven patients who survived, two patients had minor gastrointestinal bleeding with median hospital stay of 8 days with the range from 5 to 24 days, and two patients with massive pulmonary embolism died possibly due to delayed institution of catheter-directed therapy.
ConclusionCatheter-directed therapy with/without EkoSonic is an emerging alternative therapy for sub-massive and massive pulmonary embolism in children. A timely institution of catheter-directed therapy appeared important to improve the outcome.
Transcatheter therapy of anomalous systemic venous drainage
- Part of
- Shahnawaz M. Amdani, Thomas J. Forbes, Daisuke Kobayashi
-
- Journal:
- Cardiology in the Young / Volume 28 / Issue 3 / March 2018
- Published online by Cambridge University Press:
- 20 December 2017, pp. 502-506
-
- Article
- Export citation
-
Anomalous drainage of the right superior caval vein into the left atrium is a rare congenital anomaly that causes cyanosis and occult infection owing to right-to-left shunting. Transcatheter management of this anomaly is unique and rarely reported. We report a 32-year-old man with a history of brain abscess, who was diagnosed with an anomalous right superior caval vein draining to the left atrium; right upper pulmonary vein and right middle pulmonary vein draining into the inferior portion of the right superior caval vein; and a left superior caval vein draining into the right atrium through the coronary sinus without a bridging vein. Pre-procedural planning was guided by three-dimensional printed model. The right superior caval vein was occluded with a 16-mm Amplatzer muscular Ventricular Septal Defect occluder inferior to the azygous vein, but superior to the entries of right upper and middle pulmonary veins. This diverted the right superior caval vein flow to the inferior caval vein system through the azygos vein in a retrograde manner and allowed the right upper pulmonary vein and right middle pulmonary vein flow to drain into the left atrium normally, achieving exclusion of right-to-left shunting and allowing normal drainage of pulmonary veins into the left atrium. At the 6-month follow-up, his saturation improved from 93 to 97% with no symptoms of superior caval vein syndrome.
Parental anxiety among children undergoing cardiac catheterisation
- Daisuke Kobayashi, Daniel R. Turner, Thomas J. Forbes, Sanjeev Aggarwal
-
- Journal:
- Cardiology in the Young / Volume 28 / Issue 2 / February 2018
- Published online by Cambridge University Press:
- 30 October 2017, pp. 315-321
-
- Article
- Export citation
-
Background
Parents may experience anxiety and stress when their children undergo cardiac catheterisation. The goal of this study was to assess the level of anxiety in parents of children undergoing cardiac catheterisation and to identify factors that were associated with level of anxiety.
MethodsThis was a cross-sectional survey of parents of children who underwent cardiac catheterisation. Anxiety levels were measured using a validated self-report questionnaire – State-Trait Anxiety Inventory, which generates state anxiety scores on the current state of anxiety and trait anxiety scores on the stable aspects of anxiety proneness. One sample t-test was used to compare the data with normative data. Multiple linear regression was used to assess the factors associated with the state score.
ResultsA total of 113 parents completed the survey. The mean age of parents was 34.0±7.7 years and the mean age of children undergoing catheterisation was 6.7±5.7 years. Compared with normative data, mean state score was significantly higher in our cohort (p<0.05) despite no difference in the trait score. Final multivariate model showed that the state score was significantly associated with child age group (<1 year [coefficient β 7.2] and 10–18 years [6.3], compared to 1 to <10 years of age [reference]) and history of previous catheterisation (−5.2) (p<0.05).
ConclusionsConcurrent state anxiety level was high among parents of children undergoing cardiac catheterisation, whereas trait anxiety level was not. Higher anxiety was experienced by parents of infants and adolescents without a history of previous catheterisation.
Effect of Hybrid stage 1 procedure on ventricular function in infants with hypoplastic left heart syndrome*
- Daisuke Kobayashi, Girija Natarajan, Daniel R. Turner, Thomas J. Forbes, Ralph E. Delius, Henry L. Walters III, Sanjeev Aggarwal
-
- Journal:
- Cardiology in the Young / Volume 26 / Issue 5 / June 2016
- Published online by Cambridge University Press:
- 08 September 2015, pp. 867-875
-
- Article
- Export citation
-
Objective
The effect of Hybrid stage 1 palliation for hypoplastic left heart syndrome on right ventricular function is unknown. We sought to compare right ventricular function in normal neonates and those with hypoplastic left heart syndrome before Hybrid palliation and to assess the effect of Hybrid palliation on right ventricular function, using the right ventricular myocardial performance index and the ratio of systolic and diastolic durations.
MethodsWe carried out a retrospective review of echocardiographic data on 23 infants with hypoplastic left heart syndrome who underwent Hybrid palliation and 35 normal controls. Data were acquired before Hybrid and after Hybrid palliation – post 1, 0–4 days; post 2, 1 week; post 3, 2–3 weeks; post 4, 1–1.5 months following Hybrid palliation.
ResultsMyocardial performance index and ratio of systolic and diastolic durations were higher in the pre-Hybrid hypoplastic left heart syndrome group (n=23) – 0.47±0.16 versus 0.25±0.07, p<0.001; 1.59±0.44 versus 1.09±0.14, p<0.0001 – compared with controls (n=35). There was no significant change in the myocardial performance index at any of the post-Hybrid time points. Ratio of systolic and diastolic durations increased significantly 2 weeks after Hybrid – post 3: 2.08±0.62 and post 4: 2.21±0.45 versus pre: 1.59±0.44, p=0.043 and 0.003. There were no significant differences in parameters between sub-groups of infants who died (n=10) and survivors (n=13).
ConclusionsRight ventricular myocardial performance index and ratio of systolic and diastolic durations were significantly higher in infants with hypoplastic left heart syndrome before intervention compared with controls. The ratio of systolic and diastolic durations increased significantly 2 weeks after Hybrid palliation. Our data suggest that infants with hypoplastic left heart syndrome have right ventricular dysfunction before intervention, which worsens over 2 weeks after Hybrid palliation.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Blair C. Armstrong, David A. Balota, Lawrence W. Barsalou, Jos J. A. Van Berkum, Lera Boroditsky, Gregory A. Bryant, Cristina Cacciari, Joana Cholin, Morten H. Christiansen, Stella Christie, Eve V. Clark, Herbert H. Clark, Eliana Colunga, John F. Connolly, Michael J. Cortese, Seana Coulson, George S. Cree, Christopher M. Crew, Gary S. Dell, Kevin Diependaele, Judit Druks, Thomas A. Farmer, Anne Fernald, Kelly Forbes, Carol A. Fowler, Michael Frank, Stephen J. Frost, Dedre Gentner, Raymond W. Gibbs, Monica Gonzalez-Marquez, Arthur C. Graesser, Jonathan Grainger, Zenzi M. Griffin, Mary Hare, Harlan D. Harris, Marc F. Joanisse, Leonard Katz, Albert Kim, Gina R. Kuperberg, Nicole Landi, Birte Loenneker-Rodman, Danielle S. MacNamara, James S. Magnuson, Ken McRae, W. Einar Mencl, Daniel Mirman, Jennifer B. Misyak, Srini Narayanan, Kate Nation, Randy L. Newman, Lee Osterhout, Roberto Padovani, Karalyn Patterson, Kenneth R. Pugh, Terry Regier, Douglas Roland, Jay G. Rueckl, Vasile Rus, Jenny R. Saffran, Sarah D. Sahni, Arthur G. Samuel, Rebecca Sandak, Dominiek Sandra, Sophie Scott, Mark S. Seidenberg, Linda B. Smith, Michael J. Spivey, Meghan Sumner, Daniel Tranel, Gabriella Vigliocco, Nicole L. Wilson, Anna Woollams
- Edited by Michael Spivey, Ken McRae, University of Western Ontario, Marc Joanisse, University of Western Ontario
-
- Book:
- The Cambridge Handbook of Psycholinguistics
- Published online:
- 05 November 2012
- Print publication:
- 20 August 2012, pp xi-xiv
-
- Chapter
- Export citation
Databases for assessing the outcomes of the treatment of patients with congenital and paediatric cardiac disease – the perspective of cardiology
- Part of
- Kathy J. Jenkins, Robert H. Beekman III, Lisa J. Bergersen, Allen D. Everett, Thomas J. Forbes, Rodney C. G. Franklin, Thomas S. Klitzner, Otto N. Krogman, Gerard R. Martin, Catherine L. Webb
-
- Journal:
- Cardiology in the Young / Volume 18 / Issue S2 / December 2008
- Published online by Cambridge University Press:
- 01 December 2008, pp. 116-123
-
- Article
- Export citation
-
This review includes a brief discussion, from the perspective of the pediatric cardiologist, of the rationale for creation and maintenance of multi-institutional databases of outcomes of the treatment of patients with congenital and paediatric cardiac disease, together with a history of the evolution of such databases, and a description of the current state of the art. A number of projects designed to have broad-based impact are currently in the design phase, or have already been implemented. Not surprisingly, most of the efforts thus far have focused on catheterization procedures and interventions, although some work examining other aspects of paediatric cardiology practice is also beginning. This review briefly describes several European and North American initiatives related to databases for pediatric and congenital cardiology including the Central Cardiac Audit Database of the United Kingdom, national database initiatives for pediatric cardiology in Switzerland and Germany, various database initiatives under the leadership of the Working Groups of The Association for European Paediatric Cardiology, the IMPACT Registry™ (IMproving Pediatric and Adult Congenital Treatment) of the National Cardiovascular Data Registry® of The American College of Cardiology Foundation® and The Society for Cardiovascular Angiography and Interventions (SCAI), the Mid-Atlantic Group of Interventional Cardiology (MAGIC) Catheterization Outcomes Project, the Congenital Cardiac Catheterization Project on Outcomes (C3PO), the Congenital Cardiovascular Interventional Study Consortium (CCISC), and the Joint Council on Congenital Heart Disease (JCCHD) National Quality Improvement Initiative. These projects, each leveraging multicentre data and collaboration, demonstrate the enormous progress that has occurred over the last several years to improve the quality and consistency of information about nonsurgical treatment for congenital cardiac disease. The paediatric cardiology field is well-poised to move quickly beyond outcome assessment and benchmarking, to collaborative quality improvement.
Contributors
-
- By Nicholas B. Allen, Joan Rosenbaum Asarnow, Jeanne Brooks-Gunn, Ronald E. Dahl, Joanne Davila, Laura M. DeRose, Lea R. Dougherty, Nancy Eisenberg, Erika E. Forbes, Wyndol Furman, Paul Gilbert, Julia A. Graber, Danielle M. Hessler, Erin C. Hunter, Chris Irons, Lynn Fainsilber Katz, Amanda Kesek, Daniel N. Klein, Annette M. La Greca, Rebecca S. Laptook, Reed W. Larson, Primrose Letcher, Peter M. Lewinsohn, Marc D. Lewis, Christine McDunn, James W. McKowen, Christopher S. Monk, Amanda Sheffield Morris, Thomas M. Olino, Tomáš Paus, Daniel S. Pine, Ann V. Sanson, John R. Seeley, Lisa B. Sheeber, Rebecca Siegel, Jennifer S. Silk, Diana Smart, Martha C. Tompson, Julie Vaughan, Brennan J. Young, Philip David Zelazo
- Edited by Nicholas B. Allen, University of Melbourne, Lisa B. Sheeber
-
- Book:
- Adolescent Emotional Development and the Emergence of Depressive Disorders
- Published online:
- 14 September 2009
- Print publication:
- 20 November 2008, pp ix-xiv
-
- Chapter
- Export citation